Surgery - Medicover Hospital
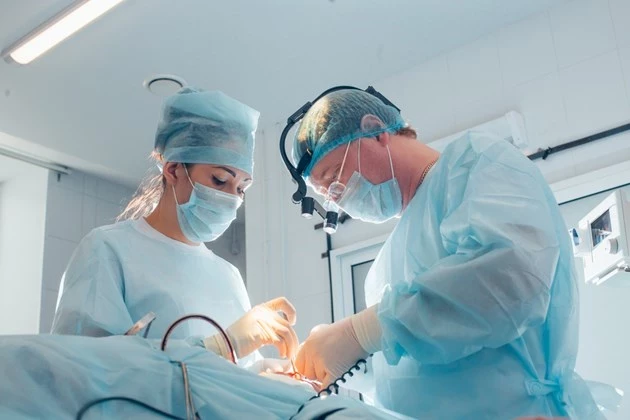
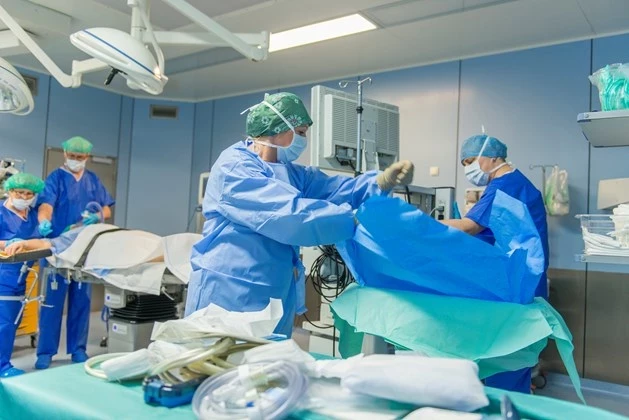
The Surgery Department of Medicover Hospital provides a comprehensive range of surgical treatments — from general and vascular surgery to oncological and plastic surgery. We use minimally invasive procedures and a modern operating theatre, which reduces pain after surgery and speeds up recovery. Safety is ensured by an experienced team of surgeons, anaesthesiologists and nurses, with care provided in a consistent path of diagnosis, treatment, and rehabilitation. The effectiveness and comfort of our procedures are confirmed by our “Hospital Without Pain” certification.
Why do patients choose us?
✔ Shorter hospitalisation times and faster recovery, ✔ Reduced risk of complications due to minimally invasive techniques and strict safety protocols, ✔ Continuous, compassionate care from specialists throughout the entire treatment process, | ✔ Advanced diagnostics, ✔ Perioperative monitoring, ✔ Individual treatment and rehabilitation plan. |
Contact us — we will answer your questions and help you plan your treatment

 Medicover
Medicover