
Over the last several decades, in highly developed countries, there has been an increase in the incidence of breast cancer, but without an increase in mortality.
Unfortunately, the disease is the third most common cause of death among women in Poland, and its cure rate is definitely lower than in other countries in the world. This is due to the fact that too few women perform preventive examinations - most cancers are detected at too advanced a stage.
The risk of developing the disease increases clearly in women over 50, and is the highest between the ages of 50 and 69. After the age of 50, mortality due to this cancer also increases.
Breast cancer metastasizes primarily to the surrounding lymph nodes, but also to internal organs, including the liver, lungs, bones or brain.
Symptoms of breast cancer
In the initial stage, no symptoms are observed. Early detection of changes is possible only by performing imaging tests.
In more advanced cases, women report to the doctor with a palpable lump in the breast. It is usually well palpable, hard, well-defined, with an uneven surface.
Where is breast cancer most often located?
The most common location of lesions is the outer, upper quadrant of the breast (35% of cases), and the least common is the lower, inner quadrant.

Characteristic symptoms of breast cancer are also:
- breast asymmetry,
- pulling in the skin or nipple,
- redness of the skin,
- skin ulceration,
- unilateral discharge from the nipple,
- enlargement of the surrounding lymph nodes on the side of the tumor,
- milkkrejectionsign may occur during lactation - the child refuses to suck the affected breast,
- breast pain - usually, when the patient feels pain, it means that the tumor is in an advanced stage and often has already metastasized.
Where does breast cancer most often metastasize?
|
Inflammatory breast cancer
A specific type of breast cancer is inflammatory cancer. In its course, the lump in the breast is small or even imperceptible. The most common symptom of inflammatory cancer is swollen, red, painful and excessively warm skin.
Inflammatory cancer is rare but has an aggressive course and is associated with a poorer prognosis.
Unfortunately, despite the preventive actions, 5-10 percent. cancer is detected too late, when there are already metastases to internal organs.
Breast cancer in men
It should be remembered that men can also suffer from breast cancer - their incidence is about 1% of all malignant breast cancers. However, unlike in the case of women, the number of breast cancer cases among men has not increased and has been more or less constant for years.
Causes of breast cancer
The cause of the development of cancer is not fully known. However, risk factors that increase the likelihood of getting the disease have been identified. The most important of them are:
- presence of gene mutations, primarily BRCA1 and BRCA2, but the risk of breast cancer may also be increased by mutations of other genes, e.g. TP53, PTEN, CHEK2, CDH1, PALPB2,
- breast cancer in close relatives, eg grandmother, mother, aunt or sister,
- a history of breast cancer,
- age over 50 - the risk of developing the disease increases with age,
- female gender - breast cancer is rare in men,
- menarche at a young age, i.e. under 12 years of age,
- late menopause, i.e. over 55 years of age,
- long-term use of menopausal hormone therapy,
- overweight and obesity in post-menopausal women,
- little physical activity,
- exposure to ionizing radiation,
- childlessness,
- late age (above 30) of having your first child,
- not breastfeeding children,
- a large amount of glandular tissue in the breasts, called high breast density,
- long-term use of oral hormonal contraceptives - this is a small increase in risk,
- a history of ovarian, endometrial or colorectal cancer,
- frequent alcohol consumption.
Not all of these factors can be influenced by a woman, so the risk of getting sick cannot be completely reduced, but even, for example, maintaining a normal body weight can have a positive effect on reducing the risk of developing breast cancer.
In addition, because some risk factors have been identified, those at higher risk may receive better prevention.
Age has a significant impact on the incidence of breast cancer in women. Women under 35 are rarely ill, and the largest group of patients are women aged 50-69. Therefore, breast cancer screening programs are targeted at women in this age group.
Is breast cancer hereditary?
The family factor is also important. In ¼ of cancer cases there is a family history of the disease (e.g. in a grandmother, mother or sister), and 5-10% are diagnosed with cancer. cases are associated with the presence of BRCA1 and BRCA2 gene mutations. The risk of developing the disease is greater, the more relatives have had cancer.
There are scales that allow an individual assessment of the risk of the disease. One of the most popular is the Gail scale. It takes into account family and medical history, the age of menarche and the age of birth of the first child. This is how 5-year and lifetime risk is assessed.
It is very important to make women aware of the factors that increase the likelihood of developing breast cancer and that women themselves can reduce this risk by changing their lifestyle, maintaining a healthy weight or regular physical activity.
Diagnosis of breast cancer
The speed of breast cancer diagnosis is crucial in terms of prognosis - the earlier it is diagnosed, the greater the chance of cure.
As part of the diagnostics, the following is performed:
- breast self-examination and breast examination by a doctor,
- mammography or breast ultrasound,
- magnetic resonance mammography,
- breast biopsy - fine-needle, core/mammotomy or surgical,
- nipple discharge test.
Diagnosis is based on microscopic evaluation of tumor tissues taken during biopsy. This examination allows to determine the type of cancer, determine the prognosis and plan the appropriate treatment.
After confirming the cancer, further diagnostics are performed to detect or exclude metastases to internal organs.
Breast self-examination
Breast self-examination plays a very important role in early diagnosis of the disease. Therefore, it is important that every woman, alone or with the help of a partner, examines her breasts according to the scheme. This test should be performed every month, preferably on the 5th-10th day of the cycle (menstruating women) or on one specific and fixed day of the month (for postmenopausal women or women who do not menstruate for other reasons).
Thanks to regular self-examination, women are able to observe even slight changes in the appearance of their breasts. If you find any abnormalities, contact your doctor as soon as possible for further diagnosis. Self-examination can save your life.
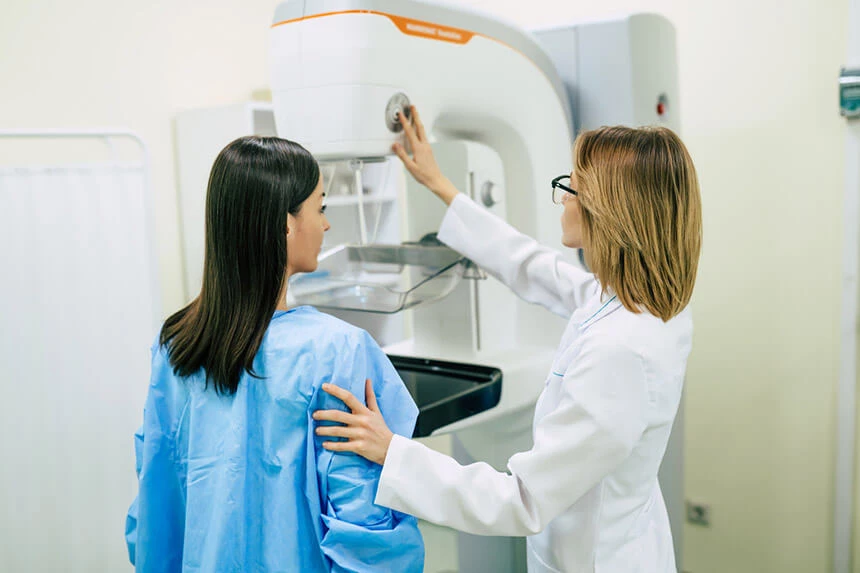
Mammography
This is important research. In Poland, the screening program covers women aged 50-69. This is the group with the highest incidence of breast cancer and high mortality rates.
In younger women, mammography is not necessarily effective because they have more glandular tissue in their breasts.
Mammography is a test that consists in X-raying the breast with a beam of X-rays. Its sensitivity1 in detecting neoplastic lesions is about 75-98%, and specificity2 reaches 52-94%. To avoid errors in the interpretation of the images, they are usually evaluated by two radiologists.
In Poland, according to the screening program, mammography should be performed every 2 years.
A correct result does not exempt you from monthly breast self-examination!
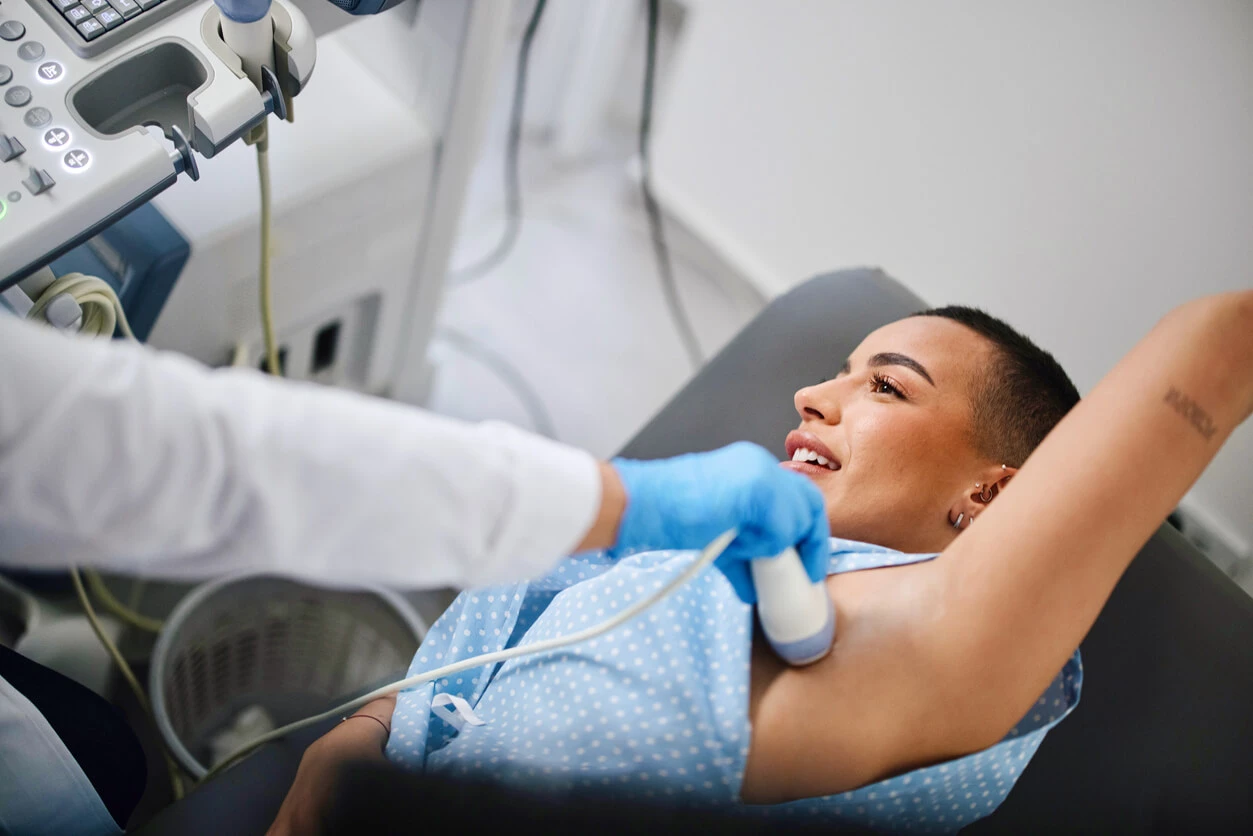
Breast ultrasound
Mammography is supplemented by breast ultrasound, which is not a screening test. Ultrasound is an important diagnostic method in young women whose breasts are dense, i.e. in the group in which mammography is less effective.
Ultrasound examination enables the differentiation of solid and cystic lesions and the determination of the nature of solid lesions - whether they are benign or suspicious. The experience of the examiner and the quality of the equipment have a great impact on the diagnostic effectiveness of ultrasound.
Magnetic resonance mammography
Magnetic resonance imaging (MR) mammography has been used more and more frequently in the diagnosis of breast cancer for several years. However, this examination is not recommended as a preventive examination for all women, but only in certain groups of patients. For several years, the American Cancer Society has recommended annual preventive screenings with this method, in conjunction with annual mammography, for women:
- in whom the estimated lifetime risk of developing breast cancer, calculated using special risk calculators based mainly on family history, is between 20 and 25% or more,
- with BRCA1 or BRCA2 mutations,
- whose first-degree relatives (parents, siblings, children) have been diagnosed with the BRCA 1/BRCA2 gene mutation,
- who underwent chest radiotherapy between the ages of 10 and 30,
- who or their first degree relatives have Li-Fraumeni syndrome, Cowden syndrome or Bannayan-Riley-Ruvalcaba syndrome.
There are several possible indications:
- resolving diagnostic doubts, if there is a discrepancy between the results of various imaging tests and/or breast examination by a doctor,
- preoperative determination of the stage or location of the cancer,
- looking for other lumps in the breasts after being diagnosed with cancer,
- checking the tightness of silicone breast implants.
The advantage of the test is its effectiveness in the case of lesions located in high-density breasts.
Breast biopsy
If the result of any of the imaging tests (mammography, breast ultrasound, magnetic resonance imaging) is abnormal, it is necessary to perform a biopsy and verify the suspicious lesion in a microscopic examination.
It can be done by various methods:
- fine needle,
- coarse needle/mammotome,
- open, also called surgical.
A fine-needle aspiration biopsy consists in puncturing a lesion previously observed in an ultrasound or mammography examination and its assessment. It is performed without anesthesia and under ultrasound guidance. The material collected in this biopsy does not distinguish between pre-invasive and invasive cancer (which may metastasize).
Core-needle biopsy is a much better test, because it allows for a full histopathological examination, determining the type of cancer, its aggressiveness and assessing the receptors: estrogen (ER), progesterone (PgR) and epidermal growth factor (HER2). This information is necessary for treatment planning. A core needle biopsy is performed under local anesthesia.
A mammotome biopsy is a type of core-needle biopsy, during which a small piece of the tumor is taken with a special device for microscopic examination.
The last type of examination, which can be used in the case of small lesions, is an open biopsy, also called a surgical one. It is performed under general anesthesia. The examination involves excision of the entire nodule with a margin of healthy tissue.
In order to assess the stage of the disease and confirm or exclude metastases, m.in. Chest X-ray or CT scan of the chest, USG or CT scan of the abdominal cavity or bone scintigraphy.
Check out Medicover's cancer diagnosis offer >>
Genetic testing for breast cancer
Genetic testing for a mutation that increases the risk of breast cancer should primarily be performed by women who:
- had at least two cases of breast or ovarian cancer in the family up to three generations ago. A particular indication is if breast or ovarian cancer appeared in the family before the age of 50,
- have already had breast or ovarian cancer, especially if the disease started before the age of 40,
- have a family member who has been diagnosed with breast cancer,
- with a family history of prostate cancer, laryngeal cancer or melanoma, in addition to breast cancer,
- who have been diagnosed with benign changes in the breasts or ovaries, e.g. cysts,
- with a family history of a BRCA1 or BRCA2 gene mutation,
- women who use hormone replacement therapy.
The genetic test is painless. It involves taking a blood sample that is analyzed in a laboratory. It takes about 7 weeks for the genetic test results.
Genetic load
However, this does not mean that a patient with a mutation in any of these genes is doomed to breast cancer. It just means he's much more vulnerable. If a mutation has not been detected in a patient, there is also no guarantee that she will not develop breast or ovarian cancer. It should be remembered that only about 20% of cancers are caused by genetic predisposition.
But what if a woman finds out she's genetically predisposed? Awareness of the increased risk of breast cancer gives a chance to include additional preventive measures or to modify their frequency. Thanks to this, we increase the chance of detecting the disease at an early stage.
We can also decide to modify our lifestyle or reduce additional risk factors:
- obesity,
- smoking, etc.
Treatment of breast cancer
The treatment regimen is always determined by a team of doctors in consultation with the patient. Such a therapeutic team includes a specialist in oncology and plastic surgery, radiotherapist, clinical oncologist, radiologist, pathologist, physiotherapist and psycho-oncologist. The general principles of cancer treatment include several basic points:
- local treatment, i.e. removal of the tumor or amputation of the breast, sentinel node biopsy and possibly removal of the axillary lymph nodes,
- radiotherapy,
- systemic treatment: chemotherapy, hormone therapy, targeted treatment (trastuzumab, lapatinib).
Surgical treatment of breast cancer
Local, i.e. surgical, treatment may be:
- breast-conserving surgery, during which the tumor is excised together with a margin of healthy tissue (additional radiotherapy is necessary after breast-conserving surgery),
- mastectomy, also known as mastectomy, which is the removal of the entire breast.
Both breast-conserving surgery and mastectomy do not differ in terms of oncological effectiveness, i.e. the length of overall survival.
The advantage of breast-conserving surgery is a better cosmetic effect and better well-being of the woman. The choice of method depends on the decision of the doctors, but it is influenced by the individual preferences of the woman.
Contraindications to breast-conserving surgery absolute:
- no possibility to carry out complementary radiotherapy,
- inability to remove the tumor with a margin of healthy tissues,
- presence of metastases in other internal organs,
- cancer recurrence after previous breast-conserving treatment.
Relative
- age of the patient below 35 years (breast cancers in such young women are usually very aggressive, so not having the breast removed significantly increases the risk of recurrence),
- a large tumor or many small nodules,
- expected bad cosmetic effect,
- the presence of disseminated microcalcifications,
- location of the tumor near the nipple,
- presence of BRCA genetic mutations.
If imaging tests and/or medical examination indicate the presence of metastases in the axillary lymph nodes, a biopsy of the suspected lymph nodes is performed. Once the diagnosis is confirmed, the axillary lymph nodes are removed during breast surgery.
If the medical examination and imaging tests do not suggest metastases in the lymph nodes, the so-called sentinel node biopsy3. The sentinel node is taken for microscopic examination and assessed for the presence of metastases.
Depending on the result of the examination, indications for the removal of axillary lymph nodes (so-called lymphadenectomy) are determined and further procedures are planned. The absence of metastases to the sentinel node allows to avoid lymphadenectomy and related complications - swelling of the hand, mobility and sensation disorders.
Radiotherapy
In the case of breast-conserving treatment, adjuvant radiotherapy is always necessary. It is aimed at destroying possible "remnants of the disease". This procedure allows to reduce the risk of recurrence of the disease and to increase the effectiveness of treatment.
Systemic treatment (chemotherapy, hormone therapy, targeted treatment)
In some cases, when the tumor is very large, treatment begins with systemic treatment, mainly chemotherapy. In some patients, chemotherapy is combined with targeted treatment, and in postmenopausal patients, initial hormone therapy is also possible.
Only later, after reducing the size of the tumor, breast-conserving surgery, amputation of the breast or radiotherapy alone is performed - it depends on the response obtained to the initial treatment.
Systemic treatment is the main treatment when the disease is generalized and metastases are present. In such situations, it is a palliative treatment, which is primarily aimed at improving the patient's quality of life.
Indications depend on many factors, including:
- the stage of the disease,
- cancer grade and type,
- the stage of the primary tumor and the condition of the axillary lymph nodes,
- presence of metastases in distant organs,
- cancer-related ailments,
- presence of symptoms that pose a direct threat to life,
- time from primary treatment to relapse,
- type of treatment used so far and its effectiveness,
- the patient's age and whether she had menopause,
- state of efficiency,
- past and coexisting diseases and their treatment,
- the patient's opinion and preferences.
Breast cancer prognosis
Cancer that is detected early and properly treated gives a chance for a complete cure. In Europe, after hearing the diagnosis, about 82 percent survive 5 years. patients, and in Poland - 72 percent. If the cancer is detected in the first stage, the percentage is 95%.
Breast cancer stages
Stage I breast cancer
The risk of death from breast cancer is very low when the tumor is less than 0.5 cm in diameter. Then the tumor grows to two centimeters.
2nd stage
The second stage of cancer development is the size of the tumor between 2 and 5 cm. Cancer cells are already in the lymph nodes in the armpit by then, and surgery is necessary. Stage II cancer development is also a situation when the tumor is smaller than 2 cm, but the cancer has invaded the lymph nodes, or it has not invaded them, but is larger than 5 cm.
3rd stage
The third stage is a tumor of any size, and the cancer has already invaded the lymph nodes and surrounding tissues - the skin of the breast or muscles.
IV stage
The fourth degree of the disease is already a very large tumor. There are already metastases to other, distant organs, e.g. bones, liver or lungs.
Prevention of breast cancer
Prevention is based on two main elements - eliminating risk factors and performing regular screening tests.
To reduce the risk of getting sick, a woman should:
- avoid long-term use of hormone replacement therapy and hormonal contraception,
- maintain proper body weight,
- be physically active for at least 150 minutes a week,
- try to have your first child before the age of 30,
- breastfeed as long as possible,
- limit alcohol consumption.
Screening tests that should be done regularly include:
- breast self-examination - all women, every month,
- mammography – women aged 50-69, every 2 years.
Women with a family history of breast, ovarian, colorectal or prostate cancer, especially in young people, should visit a genetic clinic and/or undergo genetic testing for gene mutations.
Women with BRCA1, BRCA2 or other mutations should be under constant medical supervision.
Remember!
- Check your breasts every month.
- If you notice anything worrying, contact your doctor immediately.
- If you are between the ages of 50 and 69, get a mammogram every 2 years.
Medicover offer
|
The presented medical information should not be treated as guidelines for medical conduct in relation to each patient. The medical procedure, including the scope and frequency of diagnostic tests and/or therapeutic procedures, is decided by the doctor individually, in accordance with medical indications, which he determines after getting acquainted with the patient's condition. The doctor makes the decision in consultation with the patient. If the patient wants to perform tests not covered by medical indications, the patient has the option of paying for them. |
Prezentowanych informacji o charakterze medycznym nie należy traktować jako wytycznych postępowania medycznego w stosunku do każdego pacjenta. O postępowaniu medycznym, w tym o zakresie i częstotliwości badań diagnostycznych i/lub procedur terapeutycznych decyduje lekarz indywidualnie, zgodnie ze wskazaniami medycznymi, które ustala po zapoznaniu się ze stanem pacjenta. Lekarz podejmuje decyzję w porozumieniu z pacjentem. W przypadku chęci realizacji badań nieobjętych wskazaniami lekarskimi, pacjent ma możliwość ich odpłatnego wykonania. Należy potwierdzić przy zakupie badania szczegóły do jego przygotowania. |

 Medicover
Medicover