Table of contents:
- What is colonoscopy?
- How to prepare for the colonoscopy procedure?
- After colonoscopy
- Where can you undergo colonoscopy in Warsaw?
What is colonoscopy?
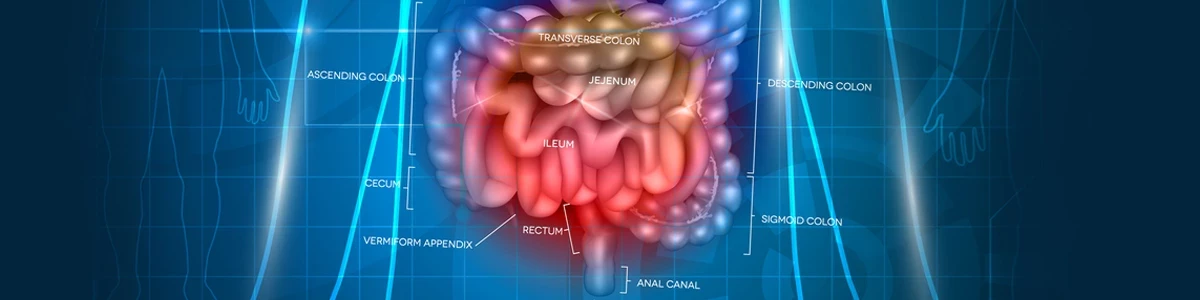
Colonoscopy is an examination that involves inserting a special device through the anus and looking at the entire large intestine. A flexible instrument called a colonoscope, 130 to 200 cm long, is used for this purpose. The visual channels in the scope allow the image of the inside of the digestive tract to be displayed at an appropriate magnification on a colour monitor. The examination is aimed to assess the surface of the colonic mucosa. With the use of additional instruments, it is possible to collect mucosal samples for histopathological examination and perform endoscopic procedures that often enable the patient to avoid surgery.
Health information to be reported to the doctor performing the examination:
- worsening of symptoms of ischaemic heart disease
- high blood pressure (hypertension)
- aortic aneurysm
- shortness of breath at rest
- bleeding tendency (haemorrhagic diathesis)
- pregnancy
- menstrual bleeding on the day of the examination
- drug allergies
- glaucoma
- mental illnesses
- any sudden discomfort during examination
- people with diabetes should make this known when registering for the examination, as in their case colonoscopy should take place in the morning. They should also consult their doctor about the preparation schedule.
Colonoscopy procedure under general anaesthesia:"I am asleep and I feel nothing"
The examination can be performed under general anaesthesia. After an intravenous injection of a sleep-inducing agent, the patient falls asleep for minutes or so and wakes up at the end of the examination. This is shallow anaesthesia and does not require the insertion of an endotracheal tube.
At the Medicover Hospital, colonoscopy is performed by experienced endoscopy specialists:
- Wojciech Kosmala MD, Endoscopy Suite Co-Ordinator, gastroenterologist
- Anna Cybulska MD PhD, gastroenterologist
- Monika Gapys MD- gastroenterologist, internist
Contact us to learn more about our offer and get more details
Call 500 900 900
or fill in the form – and we will call you back.
How to prepare for the colonoscopy procedure
Diet
- Three days before the examination: do not eat bread with grains, stone fruit (e.g. grapes, tomatoes, kiwi, strawberries), linseed, poppy seeds, sesame seeds. Pits and seeds lodged in the intestine will make it difficult to perform the examination.
- One day before the test:
- Breakfast should be easy to digest, e.g. a bun or a slice of bread and butter, cheese, hard-boiled egg, slice of cold meat, any amount of water, tea, coffee without grounds (black or with milk), clear juice.
- Between 1 pm and 3 pm you can have a creamy soup or strained broth.
- From 3 pm onwards, do not eat any more food. You can drink clear liquids: water, tea, juice, and suck on barley sweets.
- On the day of the examination:
- Do not eat any meals.
- You may drink as many clear beverages as you like, e.g. water, tea, up to 2 hours before the scheduled examination time.
Intake of the preparatory formulation
Follow the dosing schedule provided in the leaflet.
- During the preparation for colonoscopy there you will have numerous bowel movements (diarrhoea), which, towards the end, will be liquid content alone (water).
Medications
- Stop taking preparations that contain iron.
- If you are taking platelet aggregation inhibitors, consult your prescribing doctor.
- If you are taking anticoagulants, consult your doctor about anticoagulant treatment and switching to low-molecular-weight heparin.
- Continue taking your other medications as directed by your doctor, preferably 2 hours before or after taking the laxative.
After colonoscopy
- After the examination, you may experience bloating and intestinal cramps caused by air being introduced into the bowel during the endoscopy. This feeling goes away once you have passed wind.
- If you develop discomfort, such as bloating or abdominal cramps, take Espumisan (2 tablets 3 times a day) or No-Spa (tablet 3 times a day).
- After the examination, you are advised to resume your daily diet. If the examination is performed under general anaesthesia, a light diet may be eaten only from the time indicated by the anaesthetist.
- Refrain from driving or operating machines for a minimum of 12 hours after general anaesthesia, as your mental and physical performance may be impaired.
- If the examination has been done under general anaesthesia then you will remain under observation for 1–2 hours. You will need someone to drive you home after the procedure. If you do not remember the instructions your doctor gave you after the examination, contact them the next day.

 Medicover
Medicover